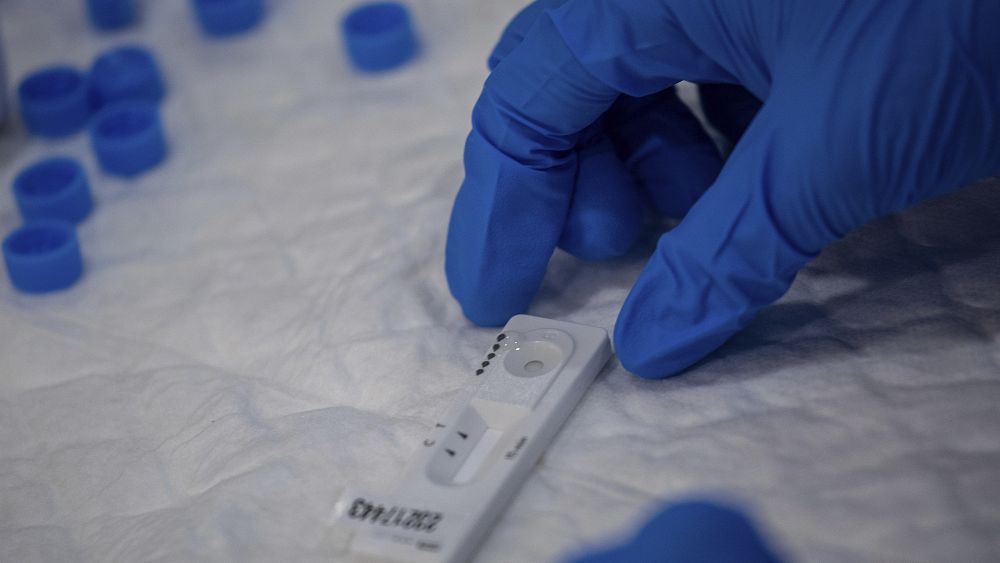
Plans to roll out 120 million rapid-diagnostic tests in the fight against coronavirus were revealed on Monday.
The tests will provide results in approximately 15 to 30 minutes, rather than hours or days, according to the World Health Organization (WHO).
The agency said the tests aimed to help lower- and middle-income countries make up ground with richer countries.
But what role could they have to play in the fight against COVID-19?
How accurate are they?
The rapid tests look for antigens, or proteins found on the surface of the virus. They are generally considered less accurate than higher-grade genetic tests, known as PCR tests.
“Those tests are pretty specific, they, like all rapid antigen tests, are not as sensitive, so you run more of a risk of a false negative, than a false positive,” Dr Gigi Gronvall, Senior Scholar at the Johns Hopkins Center for Health Security, told Euronews.
The chance of the tests giving a false negative is higher at the start of a person’s infection, according to Gronvall.
“The test will have a certain percentage of false negatives, regardless of where it’s being used and there’s also the potential for false positives,” he added.
He argued “all testing is good” but tests are just one strand in a complete approach and there has to be a strategy behind their use.
What are the benefits and drawbacks of the rapid tests?
“The speed is really the big advantage of these tests,” Gronvall said. “If it (a test) takes 48 hours to get a result sometimes, it’s like what’s the point?”
PCR tests require processing with speciality lab equipment and chemicals and have a turnaround that typically takes several days to deliver results to patients.
But the scholar argues: “There’s no reason why PCR has to take as long as it’s been taking in some places, no reason why you couldn’t have results in 24 hours or less.
“It’s just the infrastructure behind it and getting samples to where the test can be done because it is a laboratory test.”
“There are pluses and minuses with all tests, and these have the advantage of being fast and relatively easy to use and cheap, so there are lots of good things about them, but the downside is they’re not quite as sensitive as a PCR,” Gronvall explained.
“These are good tests that are a good balance between some of the positives and negatives.”
How effective are they in the fight against COVID-19 compared to PCR?
“Unfortunately, this is not an easy thing to quantify, a lot depends on how often you’re testing,” Gronvall said.
Some are arguing that PCR is “too sensitive” as they say it is detecting the virus in people before they are really contagious, he added.
“You might catch someone earlier, but because it takes longer to get results, you may miss a lot of the time when they have a lot of the virus in their nose and mouth, and they’re breathing it out,” the scholar said.
An advantage of the rapid antigen test could be that while it may not catch people with the virus when they first have it, which is probably the moment when they are not as infectious, he added.
It is rather “when you’ve got a lot of the virus in your mouth and you’re breathing it out” that you need a test to indicate that you should self-isolate.
Gronvall thinks an ideal solution would be using multiple tests for different situations, with a rapid antigen test when a result is needed quickly or there is no other option.
PCR should be used to do contact testing if there is a strong suspicion someone has been exposed because it is more accurate, he said.
“But it is more expensive, some scientists I know think we should have amped up PCR and decreased cost — there’s no reason it couldn’t be scaled theoretically,” he added.
He thinks that as more manufacturers move to roll out tests, costs may come down.
“It looks like this virus will be with us for some time, even after vaccines become available, so testing is going to have a role to play,” Gronvall said.
Source link