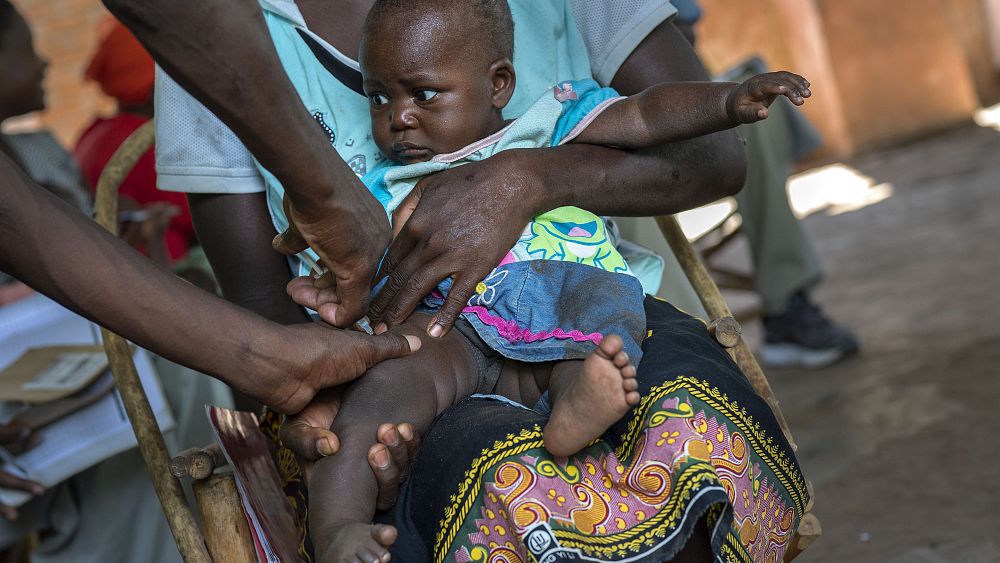
A vaccine against Malaria has been shown to be highly effective in clinical trials in Africa and could have a “major public health impact,” researchers said on Friday.
More than 400,000 people worldwide lost their lives to Malaria in 2019 — two-thirds of whom were children under the age of five, according to the World Health Organisation (WHO).
A vaccine developed by researchers from the University of Oxford was found to have a high-level efficacy of 77 per cent, becoming the first to clear the 75 per cent efficacy target set by the WHO.
It was tested on 450 children in Burkina Faso’s Nanoro department during Phase II Trials over 12 months of follow-up, with no serious adverse events related to the vaccine noted.
“These are very exciting results showing unprecedented efficacy levels from a vaccine that has been well-tolerated in our trial programme,” Halidou Tinto, Professor in Parasitology, Regional Director of IRSS in Nanoro, and the trial Principal Investigator said in a statement.
Researchers have now started recruitment for Phase III trials that will involve 4,800 children, aged 5-36 months, across four African countries.
Malaria is caused by parasites spread to people through the bites of infected female mosquitoes. The first symptoms including fever, headache, and chills, usually appear 10-15 days after the mosquito bite and can be difficult to recognise as malaria. But if not treated properly within 24 hours it can progress to severe illness and death.
Nearly half of the world’s population was at risk of Malaria in 2019, with most of the cases and deaths occurring in sub-Saharan Africa. Just six countries — Nigeria, the Democratic Republic of the Congo, United Republic of Tanzania, Burkina Faso, Mozambique and Niger — accounted for approximately half of the 2019 deaths.
Until now, the only way to protect against the disease was through insecticide, mosquito nets and antimalarial drugs, used primarily by travellers and pregnant women living in moderate-to-high transmission areas.
Adrian Hill, Director of the Jenner Institute and Lakshmi Mittal and Family Professor of Vaccinology at the University of Oxford, said that as the Serum Institute of India has committed to manufacturing “at least 200 million doses annually in the coming years, the vaccine has the potential to have major public health impact if licensure is achieved.”
Gareth Jenkins, Director of Advocacy, Malaria No More UK, also emphasised that “an effective and safe malaria vaccine would be a hugely significant extra weapon in the armoury needed to defeat malaria, which still kills over 270,000 children every year.”
“A world without malaria is a world safer both for the children who would otherwise be killed by this disease, and for us here at home. Countries freed from the malaria burden will be much better equipped to fight off new disease threats when they inevitably emerge in the future,” he added.
Source link